Parkinson’s Advanced Therapies
Introduction:
Advanced therapies for Parkinson’s disease become an option once oral medications start to cause fluctuations in response. This complication can be seen in 40% of Parkinson’s patients on long term dopamine therapy. In some these can be quite troublesome and include early wearing off of medications requiring more frequent dosing and excess movements (dyskinesias). Medication adjustments alone may not be enough to resolve these symptoms.
Advanced therapies have been available for Parkinson’s for many decades and have been shown to substantially improve motor scores and quality of life. Not all patients are suitable for these therapies and your neurologist will be able to judge this on your behalf. Each advanced therapy has its pros and cons and there is a process of education and consent prior to commencement.
The three main advanced therapies are deep brain stimulation, Duodopa® and Apomorphine. Northern Neuroscience, through its association with Hornsby Hospital is able to provide access to 2 of the main advanced therapies for Parkinson’s disease.
Apomorphine:
Despite its name, apomorphine does not contain any opioids or morphine. It is dopamine agonist type medication and is the most potent agent of this class. It is the easiest of the advanced therapies to commence and requires no procedures to initiate. It has been shown to significantly improve motor scores and dyskinesias but to a slightly lesser extent than the other advanced therapies.
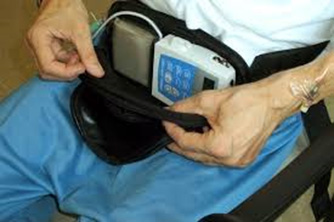
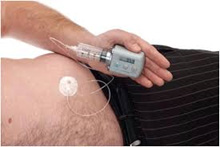
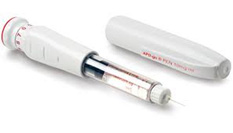
The average increase in “on” time is in the order of 2.5 hrs/ day. It has a short half life and quick onset and can be used either as a rescue medication or as a continuous pump infusion (see figure). It can only be given via a subcutaneous route as it is rapidly metabolised by the liver if given orally. Initiation requires a challenge test through the clinic/hospital to determine the optimal dose for continued therapy.
The main side effects of therapy include skin irritation, nausea, drowsiness and hypotension. It is ideal for those patients wanting to experience the benefits of an advanced therapy without committing to permanent procedures.
Duodopa®:
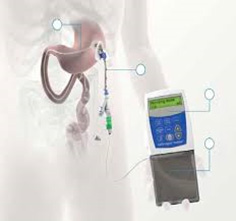
Delivering Levodopa (dopamine) directly and continuously into the gastrointestinal tract has the effect of returning dopamine levels towards a more physiological norm without the highs and lows of oral dosing. Levodopa carbidopa intestinal gel (Duodopa®) is a special formulation of dopamine that can be infused directly into the small bowel.
This therapy is highly efficacious in terms of improving motor scores, quality of life and can almost eliminate dyskinesias. The treatment effect is equal to that achieved with deep brain stimulation (DBS) surgery for Parkinson’s with an average “on” time increase of 4.5hrs/day. As opposed to DBS, It has no neuropsychological or speech related complications and can be used in a wider range of patients (i.e those that would not qualify for neurosurgery or those with cognitive impairment).
It is delivered via a system of tubing called a percutaneous endoscopic gastrostomy with jejunal (PEG-J) tube and an external pump (see figure). As it is delivered into the small intestine, it has the additional advantage of avoiding erratic absorption from delayed gastric emptying.
The main complications arise from the need for external tubing. The rate of serious complications is 5%. Complications can include infection, bleeding and blocked tubing. Most complications are seen within the first 2 weeks of tube insertion and reduce rapidly after this point. Patients are first admitted to hospital and given a trial period with the medication for 4-7 days.
This is done via a temporary tube and enables patients to experience the results prior to committing to PEG-J insertion. Close follow up is still required following initiation of therapy and is enabled via Parkinson’s community nursing.